ROCK

- Telemedicine and Health informatics
- Central MDT
- Trial MDT
- Precision medicine MDT
- Survivor support
- Prevention
- Education- CRS modules and masters in Gyn Oncology ( Tee side University, UK)
- Sarbojaya – Kolgotrg
- Contact: sarbojaya@kolgotrg.org; rock@kolgotrg.org
- Landline: +913348043706
Dedicated women’s cancer centre and ROCK – PPP model/ grant applications
The ROCK group concept:
Implementation and health care services/policy Research
– Need uniform protocol, governance, management and resources -dedicated manpower, money, time, energy: focused investment to improve ovarian cancer care
– Individuals with a common mission and vision ( operation: regional/ national/ global)
- Expert team – surgical, medical oncology, anaesthesia, super specialities, nursing, research and operations
- Volunteer medical/nursing staff
- Government – PPP model ( 2 or 3 lead sites to cater women with diverse SES)
- Donor
- Philanthropists
- Survivors and advocates
- Support from International and National centres of excellence
- Industry
Patient right to choose – centres and surgeons according to affordability but common treatment protocol, expertise and standards must be assured and ensured
- Clinical MDT
- Trial MDT
- Precision medicine MDT
Implementation steps:

- Virtual group: website
- Online and Telemedicine support: Patient information, guidance, advice on current treatment protocol, survivor group and campaigning for awareness, advocacy and treatment: visionary and missionary mode ( patient has right to choose the dedicated and trained team with repute and demonstrable track record)- emphasis-quality and survival
- Application for funding (Public and Private)
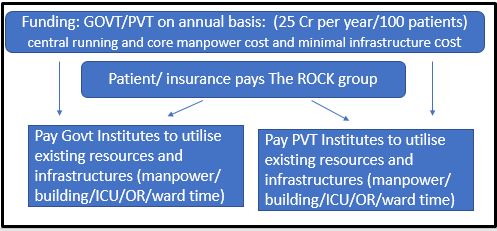
Step wise scaling up
– Institutes where The ROCK group can be housed/ infrastructures can be used on payment basis (clinical and research)
– Recruitment- volunteers and salaried
– Number of women to be seen and treated annually
– Number of outreach centres
– Education, research and training
– data science and intelligence
| High resource | Low resource | Alternative | KolGo Trg approach | |
|---|---|---|---|---|
| Optimal/ complete cytoreductive surgery | Yes, ESGO Criteria >50% Primary surgery >80% optimal CTR |
Requires Manpower resource – training and peri-op care | Most cost effective intervention | IGCS fellowship ROCK |
| Intraperitoneal chemotherapy/HIPEC | NCCN guidelines | Patchy- has cost implications | HIPEC in biological sub groups | HIPEC-HR |
| BRCA genetic testing- HBOC and prevention | Routine | Patchy- lack of genetic counsellors and tracing at risk individuals | Nurse led genetic counselling and PPI | NuGenA |
| HRD testing | Routine- costly genomic studies | Not available/ QA/ costs | Low cost academic HRD assay (Rad51) | PROVAT/ Biobanking |
| PARP inhibitors/ Avastin | Routine and Standard of care |
Not accessible/ available/ costly PFS will be different |
Intermittent / less than daily dosing/ subgroups |
IPIROC BIODIVARSITY |
| Treatment of recurrence | Trials/ targeted T/T options |
Limited options OS not prolonged |
Hormones/oral chemo/AYUSH |
HOTROC TOPARP |
| Quality of life/ Morbidity/ cost | Routine | Important but neglected end points | QAPFS/QTWIST | SOCQER-IND, HEPTROC, MOREPARP |
| Survivorship | Routine | Not well established | Snowballing | KolGo Surv/ Sarbojaya |
